7 Signs You May Need
a Root Canal
Recognizing these warning signs early can save your tooth — and significantly reduce your treatment cost. Here's what to watch for and when to act.
What are the signs you may need a root canal?
You may need a root canal if you experience: persistent tooth pain that doesn't resolve on its own, prolonged sensitivity to hot or cold lasting more than a few seconds after the stimulus is removed, swollen or tender gums near a specific tooth, tooth discoloration (gray or dark), pain when biting or applying pressure, a pimple-like bump on the gum (dental abscess), or a loose or shifting tooth. Any of these symptoms — especially if multiple occur together — warrant an exam. Learn about root canal treatment at Best Dental →
Root canal treatment often gets a bad reputation, but it's actually a tooth-saving procedure designed to relieve pain — not cause it. The problem is that most patients don't seek treatment until symptoms are severe, by which point the infection has spread further and treatment is more complex. Knowing the signs you may need a root canal early makes all the difference.
This guide covers every major warning sign, explains what's happening inside the tooth, and helps you understand when to call a dentist today vs. when you have a few days to schedule an appointment.

Persistent Tooth Pain
Ongoing tooth pain that doesn't resolve within a few days is the most common sign you may need a root canal. The pain might be constant or come and go — but the defining characteristic is that it keeps returning regardless of whether you've taken pain medication or avoided the area.
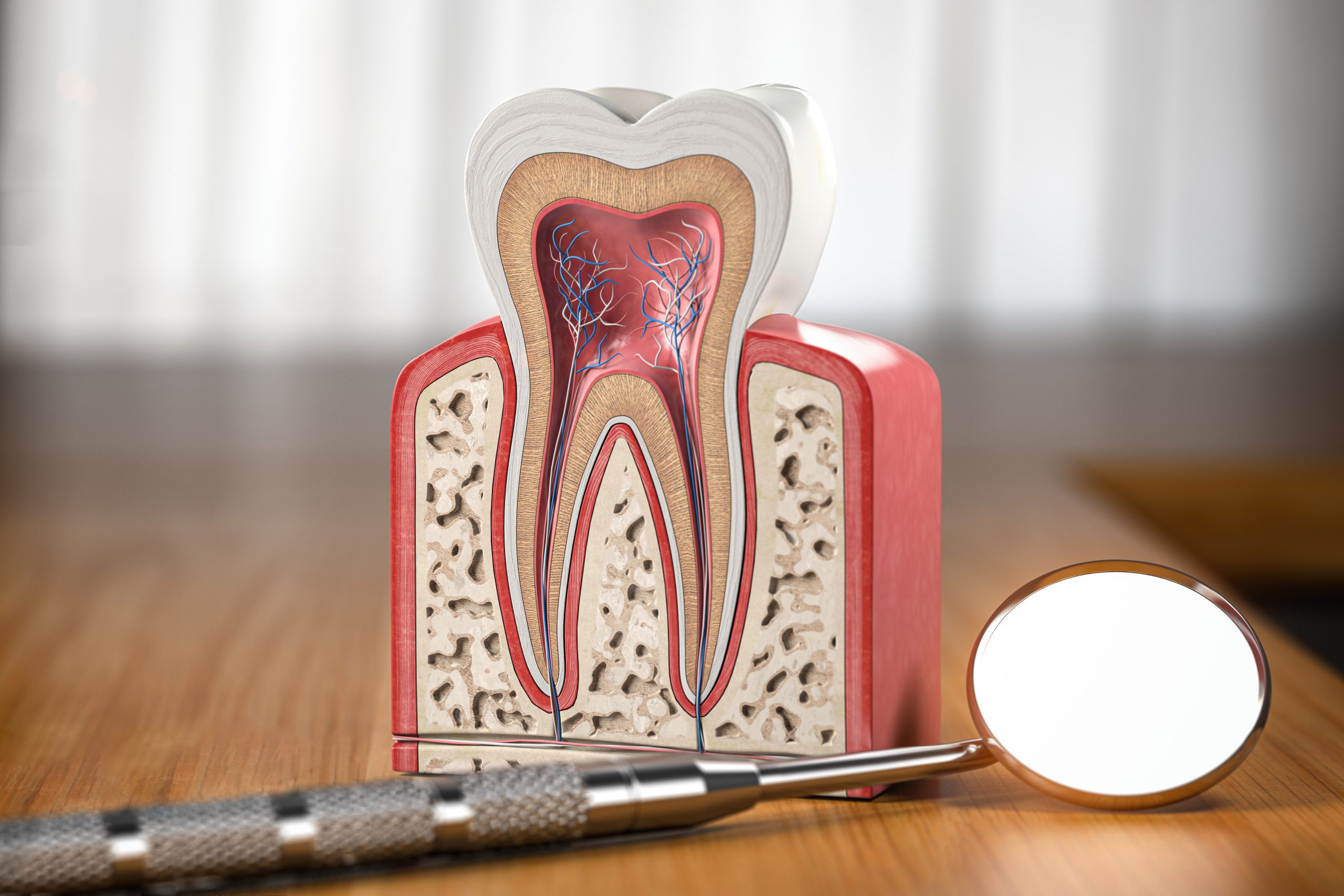
This pain occurs because the pulp inside the tooth — the soft tissue containing nerves and blood vessels — has become infected or inflamed. The pulp cannot heal itself once infection sets in, and the pressure from the infection builds inside the tooth's sealed chamber, causing the deep, throbbing ache most patients describe.
The pain may radiate to the jaw, ear, or temple on the same side of the face. Some patients mistake dental pain for a sinus headache or ear infection, delaying treatment. If over-the-counter ibuprofen provides only partial, temporary relief and the pain returns, the cause is almost certainly inside the tooth itself.
Prolonged Sensitivity to Hot or Cold
Most teeth will briefly react to extreme temperatures — a quick twinge from ice cream or a hot drink is common and harmless. What's not normal is sensitivity that lingers for several minutes after the hot or cold source has been removed.
This prolonged sensitivity signals that the pulp is inflamed or damaged. When pulp tissue becomes inflamed, it swells — but because it's enclosed inside the rigid walls of the tooth, there's nowhere for that swelling to go. The pressure amplifies the pain response to temperature changes, and the lingering sensation indicates that the nerve is significantly compromised.
Pay attention to which type of temperature triggers the response. Sensitivity to cold that lingers is a common early sign of pulp inflammation. Sensitivity to heat specifically — pain from hot liquids even when cold doesn't bother you — is a more advanced sign indicating the pulp may be partially necrotic (dying). Heat sensitivity that's relieved by cold water is a particularly urgent indicator.
Swollen or Tender Gums
Swelling around a specific tooth — along the gum line, in the jaw, or extending to the face — signals that infection has spread beyond the tooth itself into the surrounding tissues. The swelling may be accompanied by tenderness when you press on the area, and you may notice enlarged lymph nodes under the jaw or on the neck.
This swelling occurs because the bacterial infection inside the tooth creates acidic waste products that attack surrounding bone and soft tissue. As the body sends immune cells to fight the infection, inflammation and fluid accumulation cause visible swelling. This is a more advanced symptom — it means the infection is no longer contained inside the tooth.
A small, pimple-like bump on the gum near the affected tooth (called a gingival abscess or parulis) is a specific form of swelling that indicates a tooth abscess draining through the gum tissue. This bump may release pus and leave a bad taste in your mouth. It's the body's attempt to drain the infection, and while it temporarily relieves pressure, it does not resolve the underlying problem.
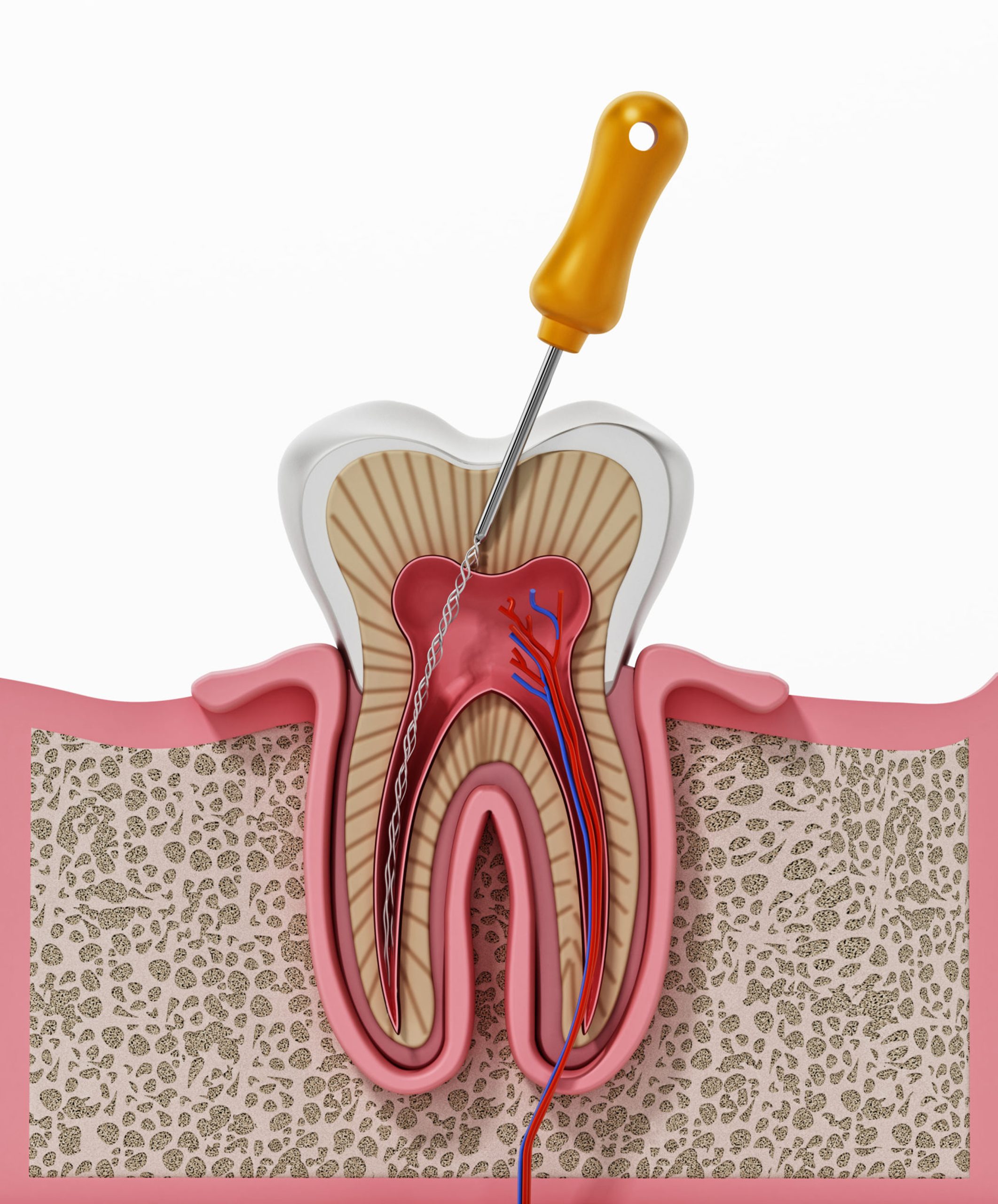
Tooth Discoloration (Darkening or Gray Tone)
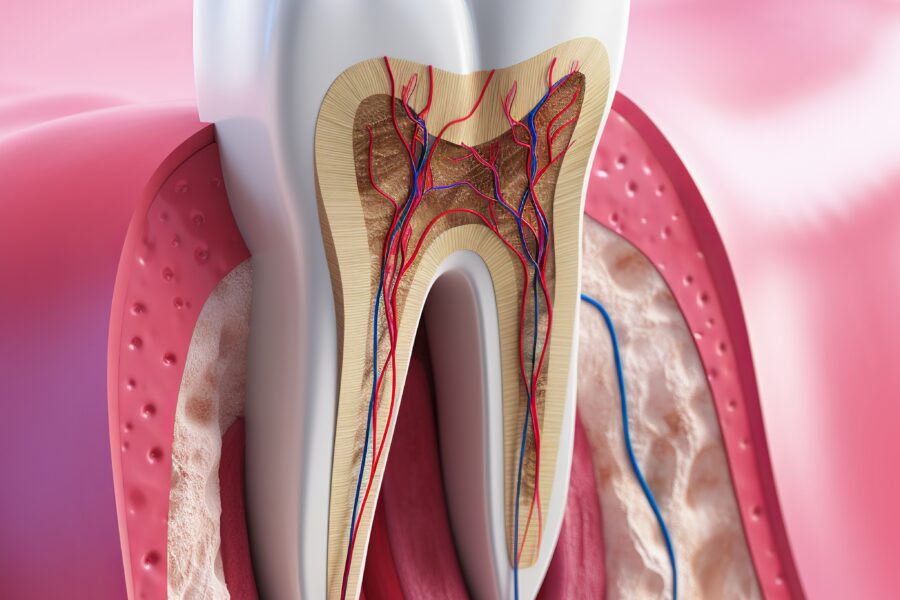
A tooth that turns noticeably darker than its neighbors — gray, brown, or black in tone — is showing signs of internal damage. This discoloration comes from the breakdown of hemoglobin in dying or dead pulp tissue. As blood cells within the pulp break down, they release compounds that stain the tooth from the inside out, and that darkness becomes visible through the enamel.
This sign is especially important because it can occur without significant pain. When the pulp dies completely, pain may actually decrease — not because the problem resolved, but because the nerve is no longer functioning. The infection, however, continues actively destroying surrounding bone tissue even in the absence of symptoms.
Tooth discoloration from internal breakdown is different from surface staining caused by coffee, tea, or tobacco. Surface staining affects all teeth somewhat uniformly and responds to whitening treatment. Internal discoloration affects a single tooth distinctly — it looks isolated and visibly different from adjacent teeth, and whitening will not resolve it.
Pain When Biting or Applying Pressure
If a tooth hurts specifically when you bite down, chew, or press on it, the infection inside the tooth has likely spread to the periodontal ligament — the thin layer of tissue connecting the tooth root to the surrounding jawbone. Once the ligament is inflamed, the tooth becomes extremely sensitive to pressure from any direction.
This sign is particularly telling because it's not triggered by temperature or spontaneous pain alone — it's mechanical. The tooth that previously felt fine under normal chewing forces suddenly becomes painful even with light contact. In some cases, the sensitivity to pressure is so pronounced that patients avoid chewing on that side entirely.
Pain on biting combined with any other sign on this list — especially persistent pain or swelling — is a strong indicator that root canal treatment is needed urgently. The combination suggests active infection that has moved beyond the pulp chamber.
A Pimple-Like Bump on Your Gum (Abscess)
A small bump — sometimes described as looking like a pimple — on the gum tissue near a tooth is a dental abscess or abscess sinus tract. This forms when the infection inside the tooth has built up enough pressure to create a drainage pathway through the bone and gum tissue. The bump may be white, yellow, or red, and pressing on it may cause it to discharge pus with a foul taste.
While the drainage may temporarily relieve the intense pressure pain, it does not resolve the infection. The bacteria causing the infection remain inside the tooth's root system, and the abscess will continue to drain — or worsen — until the source is treated. Repeated antibiotic prescriptions without root canal treatment are only a temporary measure; the infection will return.
A dental abscess is one of the clearest signs you need a root canal and among the most urgent. Left untreated, abscesses can spread infection to surrounding teeth and bone, cause permanent bone loss around the tooth, or in severe cases progress to a serious systemic infection.
A Loose or Shifting Tooth
A tooth that feels loose or has shifted in position — especially in an adult who hasn't experienced facial trauma — can indicate advanced infection that has destroyed the supporting bone structure around the tooth root. The acidic byproducts of dying pulp tissue eat away at the bone that anchors the tooth, and once enough bone is lost, the tooth loses its secure foundation.
This is typically a later-stage sign that appears after other symptoms (pain, swelling, sensitivity) have been present for some time without treatment. By the time a tooth feels loose from infection, there is usually visible bone loss on X-ray. Early root canal treatment — before bone destruction advances — offers the best chance of saving the tooth long-term.
Note that tooth looseness can also be caused by gum disease (periodontitis) rather than pulp infection. Your dentist will distinguish between these causes with a clinical exam and X-rays, as the treatment pathway differs significantly.
🚨 Go to the Dentist Today If You Have:
- Facial swelling extending toward the jaw, neck, or eye area
- Difficulty swallowing or breathing
- Fever above 101°F combined with tooth pain or facial swelling
- A dental abscess that is growing rapidly or causing vision changes
- Severe uncontrolled pain that doesn't respond to any over-the-counter medication
Root Canal Myths — Debunked
Root Canal Treatment at Best Dental — Richmond, TX
Dr. Sonny Naderi performs all root canals in-house — no specialist referral, no extra appointment. Published flat prices: