Preparing for Dental Implant Surgery
Everything you need to know before your procedure — from your first evaluation to what to stock in your kitchen the night before surgery.
Why Preparation Matters
Proper preparation doesn't just reduce anxiety — it directly influences how well your implant integrates with your jawbone and how smoothly you recover.
"Patient compliance before and after implant placement — including smoking cessation, medication management, and post-operative care — is one of the most significant modifiable factors in long-term implant success. A well-prepared patient heals faster, experiences fewer complications, and achieves better outcomes."— American Association of Oral and Maxillofacial Surgeons — Patient Preparation Guidelines
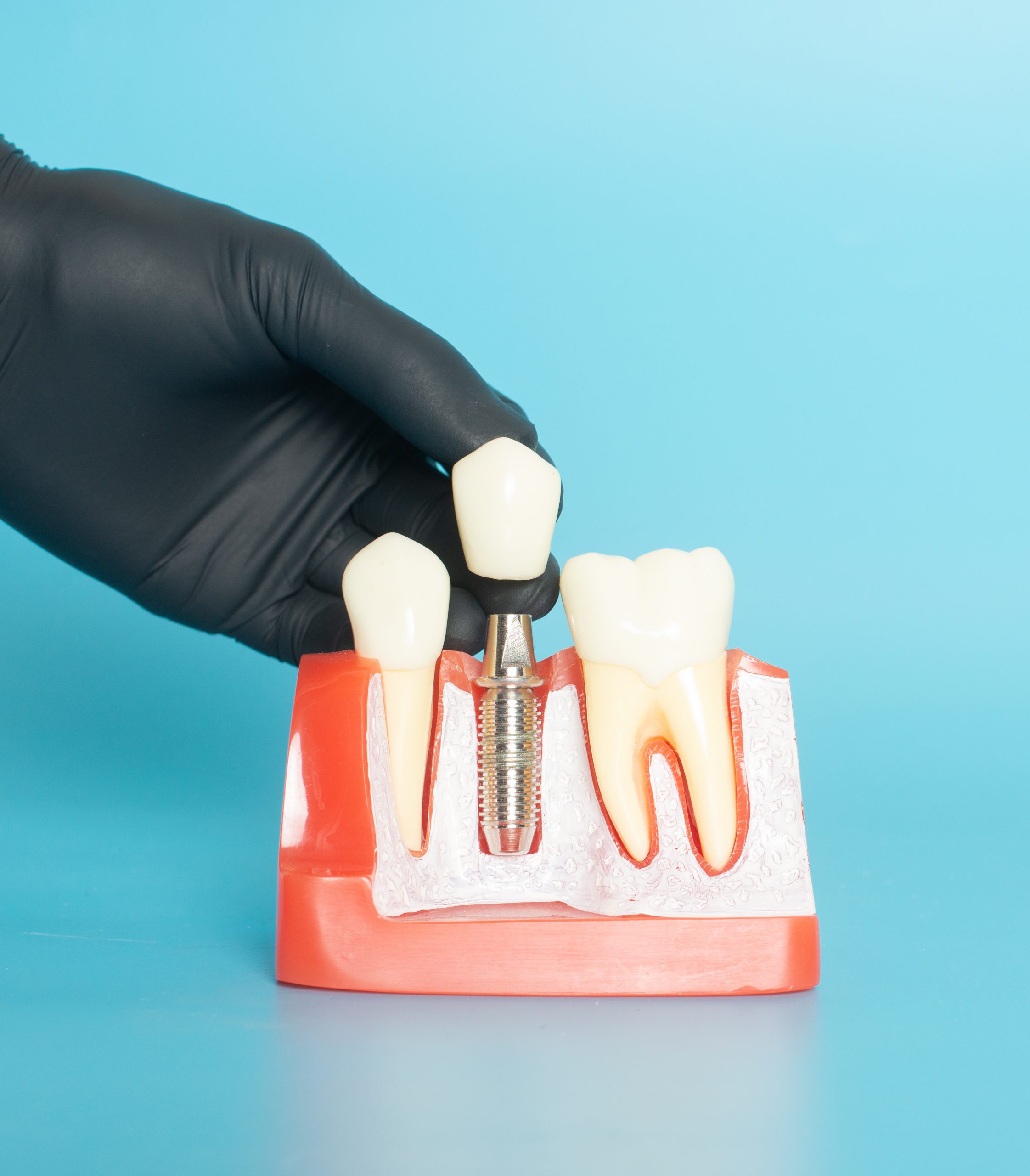
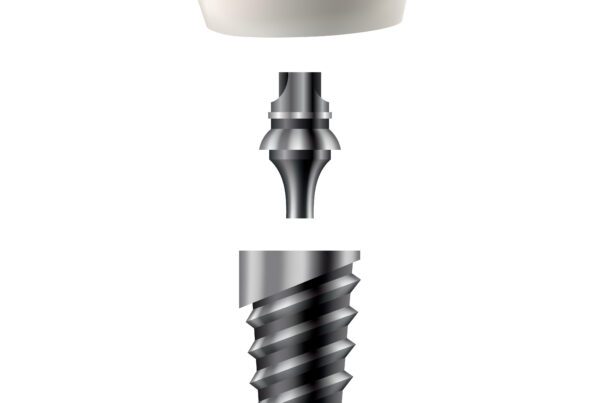
Dental implant surgery is a surgical procedure — and like any surgery, what happens in the weeks before your appointment is just as important as what happens in the chair. Your body needs to be in the best possible condition to achieve osseointegration, the biological process in which the titanium post fuses with your jawbone.
This guide covers every stage of preparation: your pre-surgical medical evaluation, medication adjustments, lifestyle changes, dietary preparation, sedation options, a complete day-of checklist, and how to set up your home for recovery. Follow these steps and you'll arrive at Best Dental calm, informed, and fully ready.
Preparation Timeline
A week-by-week roadmap from consultation to surgery day.
Initial Consultation & Treatment Planning
Meet with Dr. Sonny Naderi for a comprehensive evaluation including 3D CT imaging, bone density assessment, and full medical history review. Your treatment plan, pricing, and surgery date are confirmed. If bone grafting is needed, this is typically done 4–6 months before implant placement to allow full healing.
Lifestyle Changes Begin
Stop smoking at least 2 weeks before surgery (ideally longer). Reduce or eliminate alcohol. Begin any recommended nutritional supplementation (vitamin D, calcium). Confirm medication adjustments with both Dr. Naderi and your primary physician. Fill any pre-surgical prescriptions.
Medication Adjustments
Stop blood thinners (aspirin, ibuprofen, NSAIDs) as directed — only after physician approval. Discontinue herbal supplements that affect clotting (fish oil, vitamin E, garlic, gingko). Continue all prescription medications unless specifically told otherwise. Do not stop heart or blood pressure medications without your doctor's guidance.
Home Preparation
Stock your kitchen with soft foods for post-surgery recovery. Prepare ice packs or purchase frozen pea bags. Set up a comfortable recovery space with pillows for head elevation. Confirm your ride home and arrange work or childcare coverage for 2–3 days after surgery. Wash the loose, comfortable clothing you'll wear on surgery day.
Final Prep
If receiving sedation: stop all food and drink after midnight (or per specific fasting instructions). Shower and wash your hair — you may not feel up to it for a day or two. Lay out your clothing, insurance card, and any pre-medications for the morning. Get a full night of rest — fatigue negatively impacts healing.
Your Implant Procedure
Arrive 15 minutes early. Take any pre-medications as instructed with the smallest sip of water. Your driver should plan to stay nearby for the duration. After surgery, your recovery protocol begins immediately — ice, rest, soft foods, and prescribed medications as directed.
Pre-Surgical Medical Evaluation
Before placing any implant, Dr. Naderi conducts a thorough evaluation to confirm you're a strong candidate and identify anything that needs to be addressed first.
🩺 Medical History Review
- Current medications — prescriptions, OTC drugs, supplements
- Systemic conditions: diabetes, heart disease, osteoporosis, autoimmune disorders
- History of radiation therapy to the jaw (affects bone healing)
- Bisphosphonate use (affects bone remodeling — must be disclosed)
- Bleeding disorders or history of prolonged clotting
- Known allergies, including to metals or anesthetic agents
📡 Imaging & Diagnostics
- Cone-beam CT scan — 3D bone volume and density mapping
- Panoramic X-ray — full jaw, sinus, and nerve canal visualization
- Periapical X-rays — close-up of individual implant sites
- Digital impressions — used for treatment planning and crown fabrication
- Bite analysis — ensures implant won't be subject to excessive force
🦷 Oral Health Assessment
- Gum disease screening — active periodontal disease must be treated first
- Remaining teeth examination for infection, decay, or structural issues
- Bone quality and volume at the implant site
- Sinus proximity evaluation for upper jaw implants
- Opposing bite assessment — ensures proper occlusion with the implant crown
🩸 Lab Work (If Required)
- Blood glucose levels — elevated levels in diabetic patients must be controlled
- Clotting panel — PT/INR for patients on anticoagulants
- CBC (complete blood count) — screens for infection or anemia
- HbA1c — for diabetic patients, target below 7% for elective surgery
- Not always required — Dr. Naderi orders lab work based on your medical profile
Medication Guidance
Some medications must be paused before surgery. Never stop a prescribed medication without your physician's approval — always coordinate between Dr. Naderi and your medical provider.
| Medication / Supplement | Category | Guidance | Timing |
|---|---|---|---|
| Aspirin (low-dose) | Blood thinner | Ask your doctor — some cardiac patients should not stop | 7 days before if approved |
| Ibuprofen / NSAIDs (Advil, Aleve) | Anti-inflammatory / blood thinner | Stop before surgery | 5–7 days before |
| Warfarin / Clopidogrel (Coumadin, Plavix) | Prescription anticoagulant | Physician must approve pause — never stop without guidance | As directed by physician |
| Fish Oil / Omega-3 | Supplement — blood thinner | Stop before surgery | 1–2 weeks before |
| Vitamin E | Supplement — blood thinner | Stop before surgery | 1–2 weeks before |
| Garlic / Ginkgo supplements | Herbal — blood thinner | Stop before surgery | 1–2 weeks before |
| Antibiotics (prescribed pre-op) | Infection prevention | Take as prescribed — typically 1 hour before surgery | Morning of surgery |
| Blood pressure medications | Cardiac / antihypertensive | Continue unless told otherwise — take with small sip of water | Morning of surgery |
| Diabetes medications | Blood glucose control | Follow physician's instructions — fasting changes dosing | Coordinated with your physician |
| Bisphosphonates (Fosamax, Boniva) | Osteoporosis treatment | Must disclose to Dr. Naderi — affects implant healing; pause duration varies | Discuss at consultation |
Lifestyle Modifications
The choices you make in the weeks before surgery have a direct impact on how well your implant heals and integrates.
🚭 Smoking Cessation
- Stop smoking at least 2 weeks before surgery — ideally 4+ weeks
- Tobacco reduces blood flow to healing tissue and bone, directly impairing osseointegration
- Smokers have a 2–3x higher implant failure rate than non-smokers
- Remain smoke-free throughout the entire healing period (3–6 months)
- Nicotine patches and gums are also discouraged during healing
- Ask our team about cessation resources if you need support
🍷 Alcohol Restrictions
- Avoid alcohol for at least 48 hours before surgery
- Alcohol thins the blood, increasing bleeding risk during and after the procedure
- Alcohol interferes with anesthesia and sedation medications
- Avoid alcohol for the first week post-surgery during initial healing
- Do not consume alcohol while taking prescribed pain medications or antibiotics
🏃 Exercise & Activity
- Maintain normal activity levels in the weeks before surgery
- Avoid strenuous exercise for 48–72 hours before surgery
- Good cardiovascular health supports healing and recovery
- Post-surgery: no strenuous exercise for 3–5 days minimum
- Elevated heart rate increases swelling and bleeding risk post-op
💊 Nutritional Support
- Vitamin D supports bone health and osseointegration — discuss supplementation with Dr. Naderi
- Adequate calcium intake supports the jawbone accepting the implant
- Vitamin C supports soft tissue healing and immune function
- Stay well-hydrated in the days before surgery
- Avoid high-sugar diets that can impair immune response — especially important for diabetic patients
- Do not start new supplements within 2 weeks of surgery without approval
Dietary Preparation
Stock your kitchen before surgery day — you won't want to grocery shop with a sore jaw. Plan for soft foods for the first 5–7 days post-surgery.
✓ Soft Foods to Stock Up On
- Yogurt, cottage cheese, soft cheeses
- Smoothies and protein shakes (no straw — suction disrupts healing)
- Applesauce, mashed bananas, soft fruits
- Oatmeal, cream of wheat, soft cooked cereals
- Mashed potatoes, mashed sweet potatoes
- Scrambled eggs, soft-boiled eggs
- Soup broth (lukewarm, not hot)
- Soft-cooked fish (tilapia, salmon)
- Hummus, avocado, soft-cooked beans
- Pudding, ice cream, gelatin (avoid very cold on day 1)
- Soft-cooked pasta or overcooked rice
✗ Foods to Avoid Post-Surgery
- Hard, crunchy foods — chips, crackers, nuts, raw vegetables
- Chewy foods — steak, bagels, gummy candy, caramel
- Spicy foods — can irritate healing tissue
- Hot beverages — heat increases swelling and bleeding
- Straws — suction dislodges blood clots and disrupts healing
- Carbonated drinks — fizzing can irritate the surgical site
- Alcohol — interferes with medications and healing
- Popcorn, seeds, small particles — can become lodged in the site
- Acidic foods (citrus, tomatoes) — can irritate tissues in first days
- Very cold foods on day 1 — can cause sensitivity at the site
Sedation Options
Best Dental offers multiple levels of sedation so you can choose the comfort level that's right for you. Your sedation choice affects fasting requirements and day-of planning.
Local Anesthesia Only
The implant site is numbed with local anesthetic injections. You are fully awake throughout the procedure. No fasting required. You may drive yourself home. Best for patients who are comfortable with dental procedures and prefer to avoid sedation. Pain is fully controlled; you may feel pressure but not discomfort.
Oral Sedation
A prescription pill (typically triazolam) is taken 1 hour before the procedure, producing a relaxed, drowsy state. Combined with local anesthesia for complete pain control. You remain conscious but deeply relaxed and often have little memory of the procedure. Requires a driver. Fast from food and drink as directed.
IV Sedation
Administered directly into the bloodstream by our trained team, producing a deeper sedated state. Ideal for anxious patients, multiple implants, or complex procedures. You have minimal awareness during surgery and typically remember very little. Requires strict 8–12 hour fasting and a driver. Most predictable level of sedation comfort.
Day-of Surgery Checklist
Everything to do and bring on the morning of your procedure.
Clothing & Appearance
Wear loose, comfortable clothing with short or roll-up sleeves (for IV access if sedated). Avoid tight collars. Do not wear jewelry, nail polish, or contact lenses if receiving IV sedation. Tie back long hair. Leave valuables at home.
Fasting (if sedated)
Nothing to eat or drink for 8–12 hours if receiving IV sedation or oral sedation. You may take essential prescription medications (blood pressure, heart medications) with the smallest sip of water — ask Dr. Naderi for specific guidance at your pre-op appointment.
Pre-Medications
Take any prescribed pre-surgical antibiotics 1 hour before your appointment as directed. Take your oral sedation pill 1 hour before the procedure if prescribed. Do not take any non-prescribed medications on surgery morning without explicit approval.
What to Bring
Photo ID and dental insurance card. A list of all current medications and dosages. Any pre-surgical paperwork or forms provided by Best Dental. Your driver — who should plan to stay nearby during the procedure.
Oral Hygiene
Brush your teeth thoroughly the morning of surgery as normal. Rinse with any prescribed antimicrobial mouthwash if provided. Do not floss aggressively near extraction or graft sites if those procedures were recently performed. A clean mouth reduces bacterial load and infection risk.
Arrive Early
Plan to arrive 15 minutes before your scheduled procedure time. This allows time for paperwork, final questions, and getting settled — arriving stressed or rushed is not the ideal start to a surgical procedure. Let your driver know the expected duration (typically 1–3 hours depending on complexity).
Setting Up for Recovery
Prepare your home before surgery day — you'll be glad you did when you get back. The first 24–48 hours are the most important for managing swelling and discomfort.
Ice Packs Ready
Have 2–3 ice packs or zip-lock bags of frozen peas in the freezer. Apply to the outside of the face (not directly on skin — wrap in a cloth) for 20 minutes on, 20 minutes off for the first 24 hours. Ice significantly reduces post-surgical swelling. After 48 hours, switch to warm compresses.
Prescriptions Filled Before Surgery
Fill all post-surgical prescriptions before your procedure — typically pain medication and antibiotics. You won't want to stop at a pharmacy on the way home. Take the first dose of antibiotics before swelling and discomfort make it easy to forget. Dr. Naderi prescribes antibiotics for most implant surgeries to prevent infection.
Elevated Rest Setup
Keep your head elevated above your heart for the first 24–48 hours — this reduces swelling and bleeding. Set up pillows to prop yourself up while sleeping. Avoid lying completely flat. A recliner is ideal if you have one. Have entertainment (phone, TV remote, book) within reach so you don't have to get up unnecessarily.
Soft Food Kitchen Stocked
Refer to the dietary preparation section above and shop 2–3 days before surgery. You'll be eating soft foods for 5–7 days, so stock enough for at least a week. Prepare some items in advance (mashed potatoes, oatmeal) so they're ready without cooking effort post-surgery. Keep everything at room temperature — not hot or very cold initially.
Time Off Work & Childcare
Plan for 2–3 days away from work for most single-implant procedures. Full-arch or complex cases may require 4–5 days. If you have young children, arrange childcare support for the first 48 hours — you should not be lifting, bending, or exerting yourself. Notify your employer ahead of time so there's no scheduling pressure to return before you're ready.
Oral Care Supplies
Purchase a new soft-bristled toothbrush before surgery — you'll need to switch to gentle brushing around the surgical site. Have a bulb syringe (irrigation syringe) available if recommended by Dr. Naderi for site flushing later in healing. Saltwater rinses begin 24 hours post-surgery; have salt on hand. Do not use commercial mouthwash containing alcohol — it disrupts healing.
Best Dental's Contact Saved
Save (281) 215-3065 in your phone before surgery. Most post-surgical questions can be answered by our team quickly. Contact us immediately if you experience excessive bleeding (soaking through gauze after 1–2 hours), fever above 101°F, severe increasing pain after day 3, or visible movement of the implant.
Your Surgeon at Best Dental
Dr. Sonny Naderi — Fellowship-Trained Oral Surgeon & Implant Specialist
Dr. Sonny Naderi brings over 20 years of surgical experience and more than 25,000 procedures to every implant case. Fellowship-trained in oral surgery, Dr. Naderi uses 3D cone-beam CT imaging and computer-guided placement technology to maximize precision and minimize recovery time. His thorough pre-surgical consultations ensure every patient arrives prepared, confident, and clear on what to expect — from the first appointment through full osseointegration.
Learn More About Dr. Sonny Naderi →Frequently Asked Questions
Common questions patients ask before their implant surgery at Best Dental.
Key Takeaways — Preparing for Implant Surgery
Related Resources
More from Best Dental on implants, pricing, and care.
Ready to Take the Next Step?
Schedule a consultation with Dr. Sonny Naderi at Best Dental in Richmond, TX. We'll walk you through your complete treatment plan, answer every question, and make sure you arrive on surgery day fully prepared and confident.